Dr Petra's Blog
You may remember before Christmas there was a lot of media attention to new research from Africa that suggested men who had been circumcised had lower HIV rates than men who had not undergone this procedure. I had a few questions about the research - particularly why it was a halted trial that went straight to media rather than being published anywhere.
Other colleagues working in the area of HIV have raised more specific concerns about the HIV/Circumcision research and the issues it raises. In particular there are worries that a population that’s not particularly health literate may interpret the study as circumcision gives immunity from HIV, and also that this research doesn’t include the health of women.
One such colleague, David Gisselquist*, has provided some thoughtful analysis of this latest research. He has kindly allowed me to reproduce his views on the HIV/Circumcision trial here:
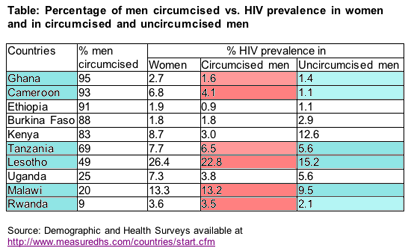
“Three prospective studies report that circumcision protects African men from sexual acquisition of HIV. What is going on is not so clear. If circumcision is so protective, then why do CIRCUMCISED men in 6 of 10 African countries have HIGHER HIV prevalence than uncircumcised men in Demographic and Health Surveys (see attached table)? If circumcision protects men from sexual acquistion of HIV (and that may be so), then data on HIV prevalence suggests that most HIV in men in Africa is coming from something else.
Table showing HIV prevalence and circumcision
High HIV incidence and prevalence in women, especially young women, almost defines Africa’s HIV epidemic. So let’s look at HIV in women vs. male circumcision (see table above). If we consider countries in Southern Africa in a group, and all other countries in Africa as another group, we find:
The African AIDS literature is awash in fantasies about sugar daddies, and no doubt there are some. But what about risks during gynecological and antenatal care? If researchers in Europe had not looked at blood risks for groups of European women with 20%-50% HIV prevalence, but just winked and implied that the women were promiscuous (and lied about it), the researchers would be recognized as incompetent and probably anti-female. But AIDS experts get away with that sort of behavior in Africa.
Some specific questions that have been avoided for decades: Are multidose vials of tetanus contaminated? What happens to women when specula are reused without sterilization? Is equipment used to draw venous blood during antenatal care sterile? What about conditions during delivery?
When is safe health care for women in Africa going to be a priority in AIDS prevention? Circumcising men will not make women’s health care safe”.
*David is an anthropologist and economist and co-runs a listserve called RELASH (REporters and LAwyers for Safe Healthcare). RELASH is looking for reporters, lawyers, and others interested to share ideas about how to respond to unexplained HIV infections - to promote investigations, compensation and change.
January 7, 2007
I'm Dr Petra, and my
blog covers sex and relationship issues
that matter
|